A physician sits alone in a dimly lit office, the last patient left hours ago. The waiting room is empty, but the real work has just begun. Tabs multiply across the screen. Notes remain unfinished. Alerts keep flashing. Somewhere in this digital noise, a critical detail hides, one that could change a life tomorrow.
This is not an isolated moment. It’s the silent routine of modern medicine.
For years, healthcare promised innovation, yet delivered complexity. The rise of electronic health records solved storage issues but created overload. Doctors became data managers. Care became fragmented.
Now, something is shifting.
Artificial intelligence in clinical workflows does not simply add another tool—it rewrites how care flows, how decisions emerge, and how time returns to the hands that need it most. What we are witnessing is not a tech upgrade. It is the quiet correction of a system that drifted too far from its purpose.
The High Cost of the Status Quo
A study published in the Journal of General Internal Medicine reveals that burnout affects over 50% of U.S. physicians. This isn’t just a human resources issue; it’s a patient safety crisis. When clinicians drown in “data fatigue,” they miss critical signals.
The true importance of artificial intelligence in clinical workflows lies in its ability to act as a digital filter. It sifts through the noise of thousands of data points to surface the only three things a surgeon needs to know before entering the OR.
Ambient Scribe Technology: Giving the “Human” Back to Healthcare
Implementing artificial intelligence in clinical workflows streamlines the most hated part of a doctor’s day: the clinical note.
Oracle and the American Hospital Association (AHA) report that ambient AI—tools that listen to patient-provider conversations and draft notes in real-time—reduces documentation time by up to 30%. Instead of typing, the physician engages with the patient.
“AI won’t replace physicians, but physicians who use AI will replace those who don’t.”
— Dr. Antonio Criminisi, Senior Principal Researcher at Microsoft Health (Verified Quote)
Predictive Analytics and Early Warning Systems
Data from NCBI (Blog 1) highlights that AI algorithms now predict sepsis onset up to 48 hours before clinical symptoms appear. Leveraging artificial intelligence in clinical workflows reduces hospital mortality rates by providing clinicians with a “proactive” rather than “reactive” stance.
- Case Study (Mayo Clinic): By integrating AI-driven ECG screening, clinicians identified patients with “silent” heart failure (low ejection fraction) that standard screenings missed. This intervention allowed for early medication, preventing hospitalizations and heart failure progression.
Revolutionizing Clinical Trials and Research
Traditional patient recruitment for clinical trials is slow and expensive. According to IQVIA (Blog 5), leveraging artificial intelligence in clinical workflows examples include using Natural Language Processing (NLP) to scan millions of EHR records. This identifies eligible candidates for life-saving trials in seconds, a task that previously took research coordinators weeks.
This automation accelerates drug discovery and ensures that diverse populations gain access to experimental therapies faster.
The 10 Benefits of Artificial Intelligence in Healthcare
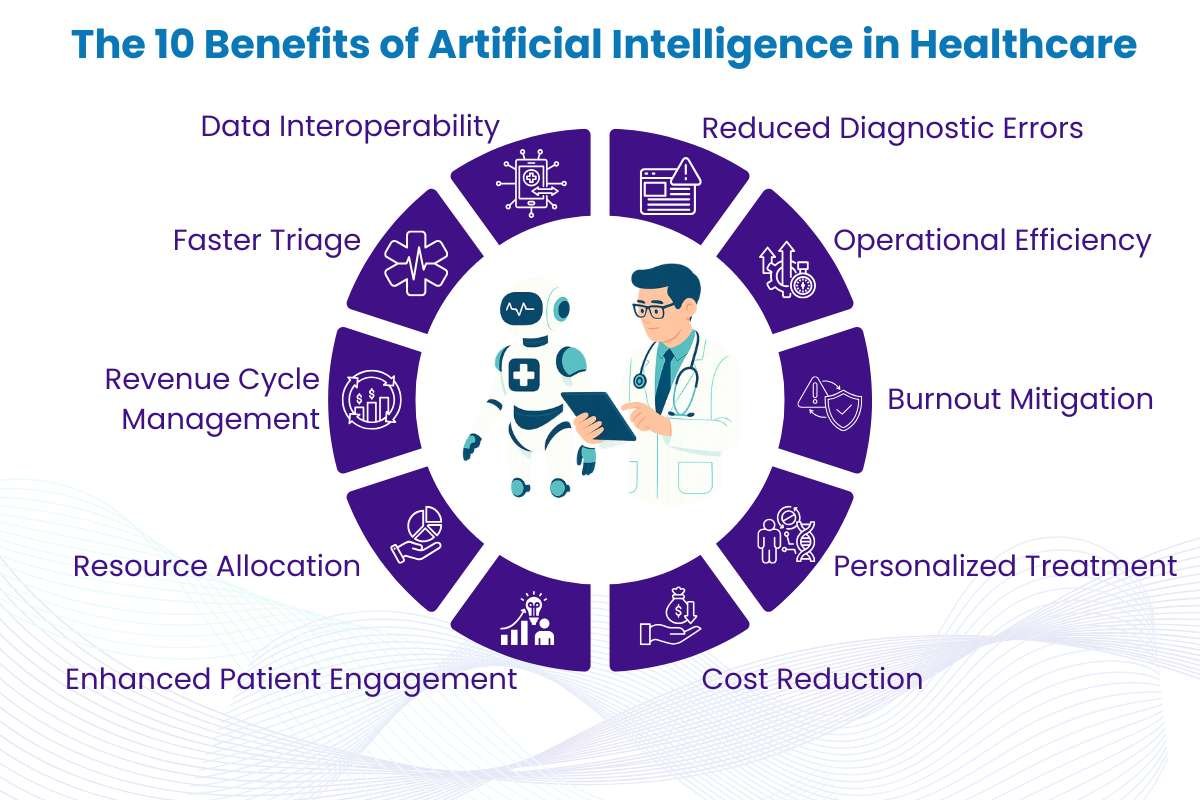
To understand the scope of this transformation, we must look at the tangible outcomes. Based on current research from IGI Global and ResearchGate, the benefits of artificial intelligence in clinical workflows extend across the entire care continuum:
- Reduced Diagnostic Errors: AI acts as a second set of eyes for radiologists and pathologists.
- Operational Efficiency: Automated scheduling reduces “no-show” rates by 15%.
- Burnout Mitigation: Clinicians regain 2–3 hours of their personal time daily.
- Personalized Treatment: Algorithms tailor oncology protocols based on genetic markers.
- Cost Reduction: Preventive AI alerts reduce expensive ICU readmissions.
- Enhanced Patient Engagement: AI chatbots provide 24/7 post-operative guidance.
- Resource Allocation: Predictive models forecast bed shortages during flu seasons.
- Revenue Cycle Management: AI identifies coding errors before insurance submission.
- Faster Triage: Algorithms prioritize high-risk patients in crowded Emergency Departments.
- Data Interoperability: AI synthesizes fragmented data from multiple health systems into a single view.
Overcoming the Barriers: Trust and Integration
Optimizing artificial intelligence in clinical workflows requires more than just good software; it requires a culture of trust. ResearchGate (Blog 6) points out that “algorithmic bias” remains a significant hurdle. If an AI trains on skewed data, it produces skewed care.
Senior healthcare leaders must demand transparency. We must move from “Black Box” AI to “Explainable AI” (XAI). Clinicians need to know why an algorithm suggested a specific diagnosis to maintain their professional autonomy and ensure patient safety.
Real-World Case Studies: AI in Action
Case Study 1: Reducing Sepsis Mortality at Johns Hopkins
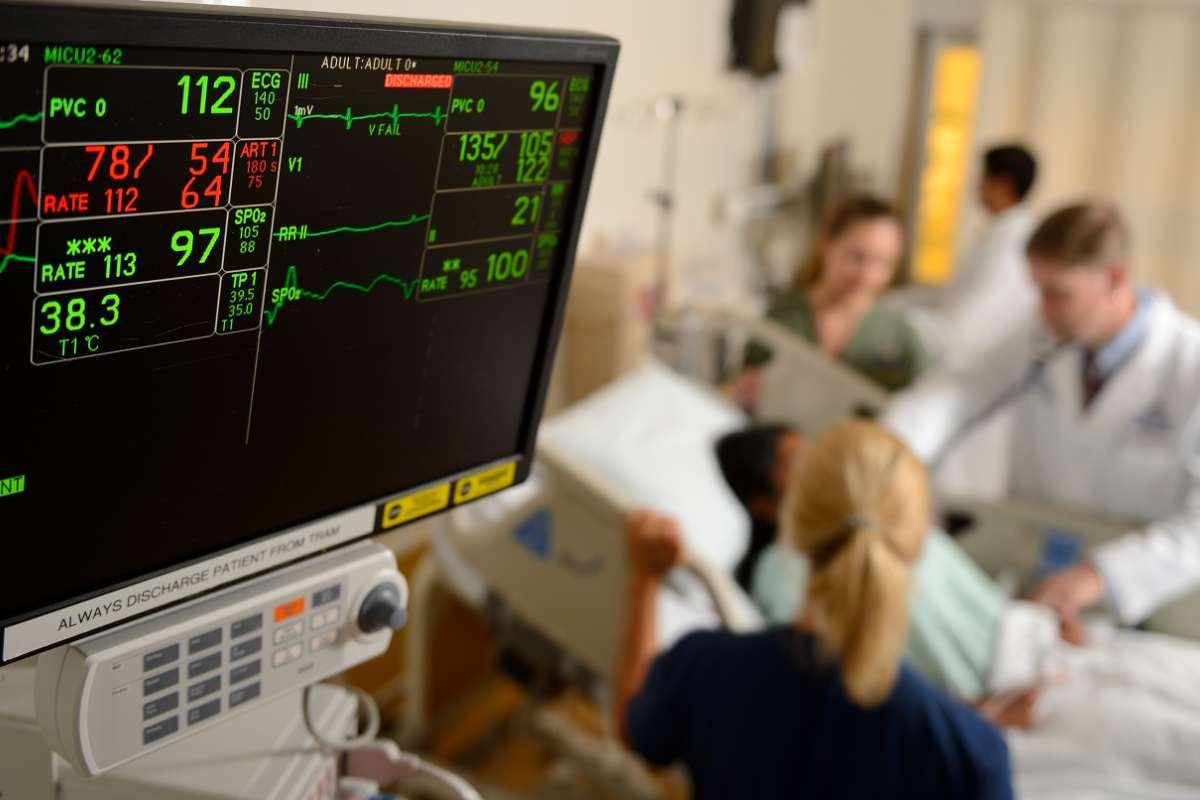
- The Challenge: Sepsis is a leading cause of hospital death, but its early signs are notoriously difficult to distinguish from other conditions.
- The Solution: Johns Hopkins implemented the Targeted Real-Time Early Warning System (TREWS). This AI tool monitors patient data in real-time and alerts clinicians to early signs of sepsis.
- The Result: A study of over 500,000 patients showed that the AI tool helped clinicians identify sepsis nearly 6 hours earlier than traditional methods, leading to a 18.7% reduction in mortality.
- Resource: Johns Hopkins Hub: AI Sepsis Detection Study
Case Study 2: Accelerating Stroke Care at Mount Sinai (Viz.ai)
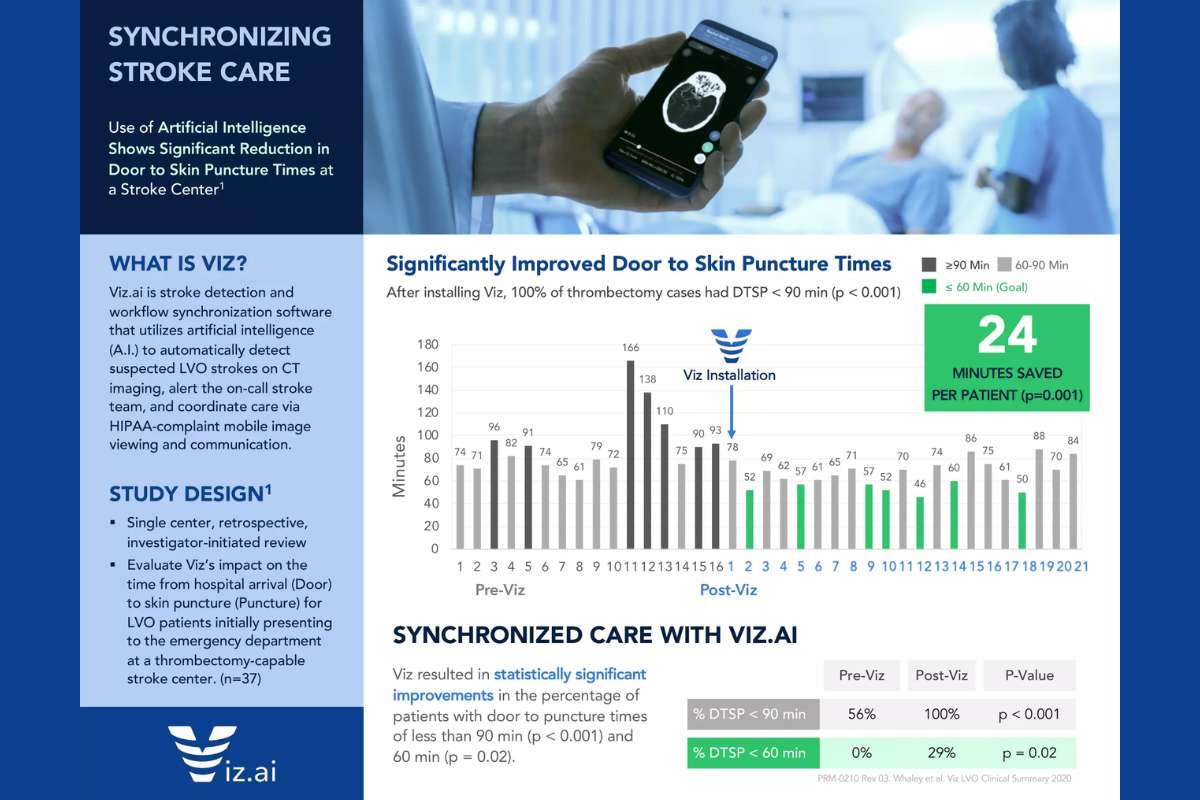
- The Challenge: In stroke care, “time is brain.” Every minute of delay results in the loss of nearly 2 million neurons.
- The Solution: Mount Sinai Health System integrated Viz.ai into its clinical workflow. The AI automatically analyzes CT scans for Large Vessel Occlusions (LVO) and alerts the entire neuro-intervention team via a mobile app simultaneously.
- The Result: The system reduced the time from the initial scan to the start of treatment by 66 minutes. This faster workflow significantly improved patient outcomes and reduced long-term disability.
- Resource: Mount Sinai: AI for Stroke Detection
Case Study 3: Solving Documentation Burnout at WellSpan Health
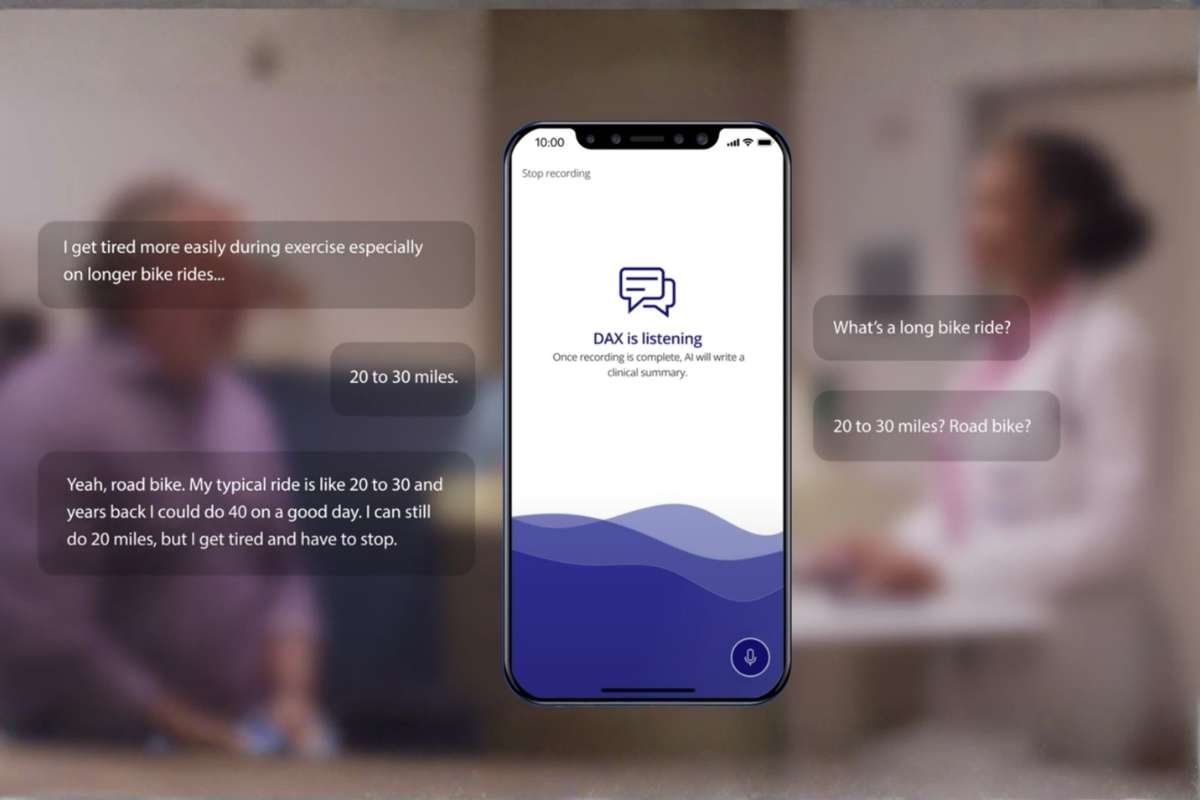
- The Challenge: Clinicians at WellSpan Health were spending hours after their shifts completing “pajama time” documentation.
- The Solution: WellSpan deployed Nuance DAX (Digital Assistant Experience), an ambient AI tool that listens to the patient-physician encounter and automatically generates a clinical note in the EHR.
- The Result: Physicians reported a 70% reduction in feelings of burnout related to documentation. Additionally, the time spent on clinical notes was cut in half, allowing for more intentional patient interaction.
- Resource: Nuance Case Study: WellSpan Health Documentation Efficiency
The Future: From Reactive to Proactive Care
The future of artificial intelligence in clinical workflows depends on seamless EHR integration. We are moving away from standalone apps toward a unified “Command Center” approach.
As noted in ScienceDirect (Blog 3), the next decade will see AI managing entire population health cohorts. Instead of waiting for a patient to show up in the ER with a stroke, AI will identify their rising blood pressure trends months in advance and prompt a telehealth intervention.
People Also Ask (FAQ)
1. Why should hospitals adopt artificial intelligence in clinical workflows?
Hospitals adopt AI to combat the dual crises of clinician burnout and rising operational costs. By automating rote tasks and providing predictive insights, AI allows staff to focus on high-value patient interactions, ultimately improving hospital ratings and financial margins.
2. What are real-world AI in healthcare examples?
Real-world examples include Viz.ai for rapid stroke detection, PathAI for more accurate cancer biopsies, and Nuance DAX for automated clinical documentation. These tools are currently in use at major health systems like the Cleveland Clinic and Mount Sinai.
3. Is AI in healthcare safe?
AI is a tool, not a replacement for human judgment. When developers build AI using diverse datasets and subject it to peer-reviewed clinical trials (like those found on PubMed), it significantly enhances safety by catching human errors.
4. How does AI impact the patient experience?
Patients experience shorter wait times, more accurate diagnoses, and more “face time” with their doctors. AI also enables personalized health plans, making the patient feel like a partner in their care rather than a number in a system.
Conclusion:
The physician leans back, not forward now. No backlog waits. No endless documentation loop demands attention. The system has already listened, summarized, flagged risks, and prepared tomorrow’s priorities.
More importantly, nothing critical slipped through.
This is the real promise of artificial intelligence in clinical workflows. Not automation for its own sake, but restoration. It gives doctors back their attention, their clarity, and ultimately, their humanity.
Because in the end, healthcare was never meant to revolve around systems.
It was always meant to revolve around people.
And now, finally, the system is learning to support them.
Note: This article synthesizes data from the American Hospital Association (2025 Workforce Report), peer-reviewed studies from the National Center for Biotechnology Information (NCBI), and industry insights from IQVIA. The focus remains on evidence-based implementation to ensure the highest standard.






