Imagine your body’s security system suddenly starts a riot. Instead of patrolling the hallways to catch a small leak, every guard in the building dumps all the world’s concrete onto the floor at once. Now, you have massive blockages stopping traffic. Even worse, when a real pipe bursts elsewhere, you have no concrete left to fix it.
This internal chaos explains exactly what is disseminated intravascular coagulation. It is a rare, life-threatening condition where your blood’s clotting process goes rogue. Often known as the “death is coming” syndrome in medical circles, though its clinical name is DIC.
In this updated guide, we break down the mechanics, symptoms, and the latest 2025 medical standards for managing this crisis.
The Simple Definition: What is Disseminated Intravascular Coagulation?
At its core, disseminated intravascular coagulation is a massive imbalance. Normally, your blood stays liquid until you get a cut. Then, proteins called “clotting factors” rush to the scene to plug the hole.
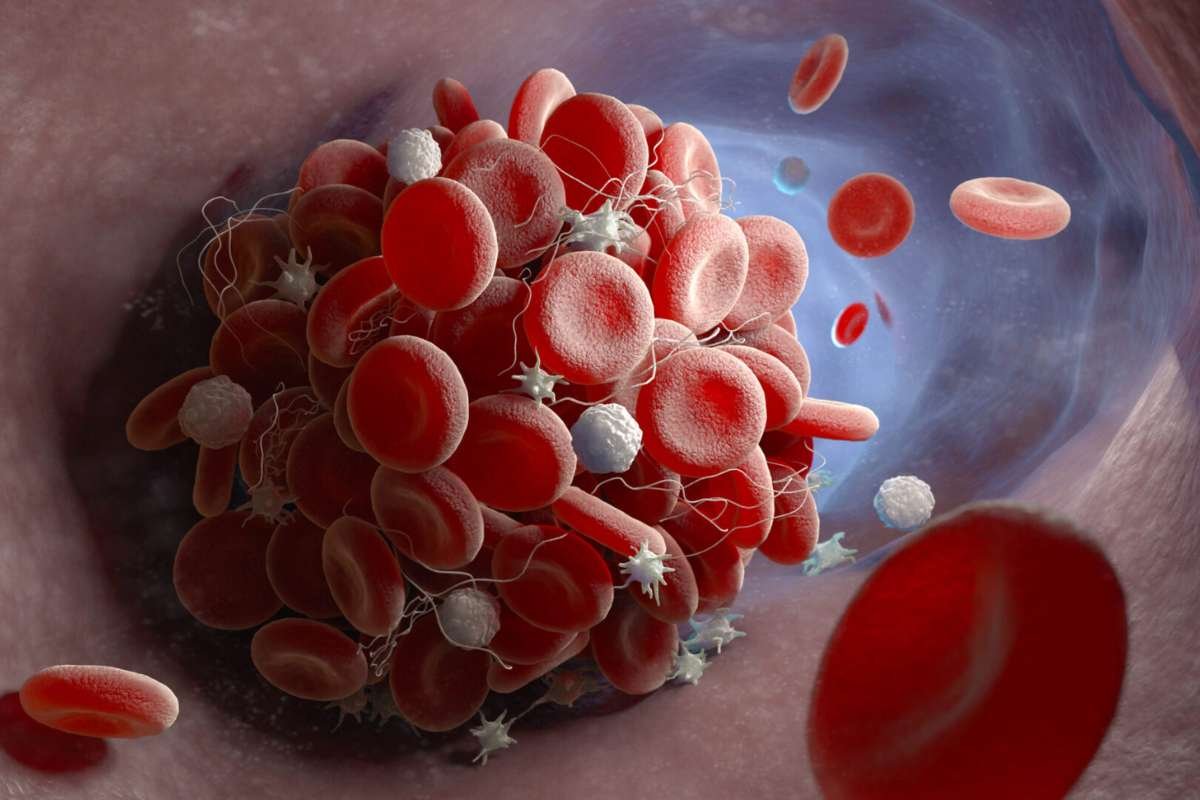
In DIC, an underlying illness, like a severe infection or cancer, triggers these proteins to activate everywhere in your body. This creates thousands of tiny clots in your small blood vessels. These clots act like tiny road dams. They stop oxygen from reaching your kidneys, liver, and lungs.
Because your body uses up all its “glue” (platelets and clotting factors), making these tiny useless clots, you start to bleed from other places. You might bleed from your gums, your nose, or even where an IV entered your skin.
Comparison: Acute vs. Chronic DIC
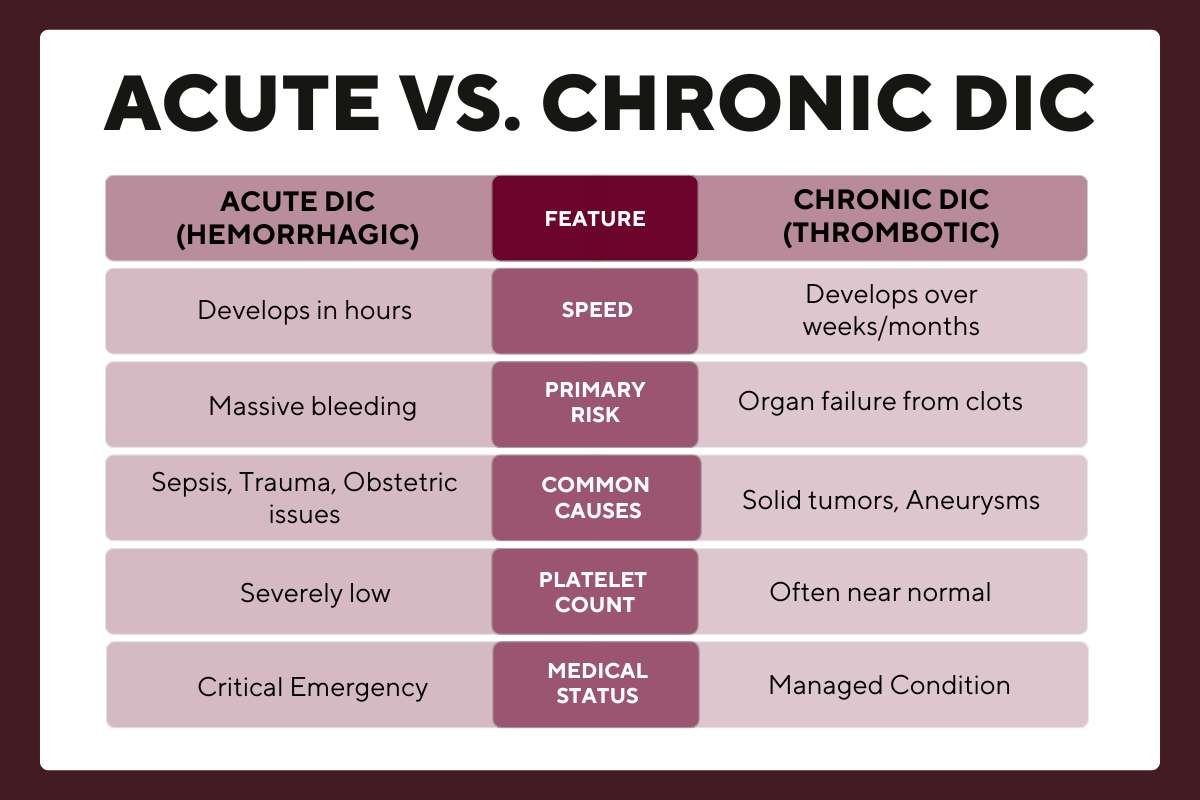
Not every case looks the same. Depending on the speed of the trigger, the body reacts differently.
| Feature | Acute DIC (Hemorrhagic) | Chronic DIC (Thrombotic) |
| Speed | Develops in hours | Develops over weeks/months |
| Primary Risk | Massive bleeding | Organ failure from clots |
| Common Causes | Sepsis, Trauma, Obstetric issues | Solid tumors, Aneurysms |
| Platelet Count | Severely low | Often near normal |
| Medical Status | Critical Emergency | Managed Condition |
Understanding these differences helps doctors answer what is disseminated intravascular coagulation for each specific patient.
Why Does the Body Panic? (The Triggers)
Understanding disseminated intravascular coagulation requires looking at the “spark” that starts the fire. DIC never happens on its own; it always follows another serious health event.
- Severe Sepsis: Sepsis triggers nearly 35% to 50% of all DIC cases. Bacteria in the blood send your immune system into a tailspin.
- Cancer: Up to 20% of patients with advanced cancers like leukemia or solid tumors develop chronic DIC.
- Childbirth Complications: Conditions like placental abruption or HELLP syndrome can suddenly shift the body into a hyper-clotting state.
- Trauma: Major injuries or burns release “tissue factor” into the blood. This acts like a match in a gasoline-soaked room.
The Statistics: Why We Must Act Fast?
Data from the National Center for Biotechnology Information (NCBI) shows that mortality rates for sepsis patients double if they develop DIC. Recent reports from 2025 suggest the global market for DIC treatments grows by 5.3% annually. This reflects how often doctors now encounter this condition in aging populations.
“DIC is not a single disease. It is a dynamic process where the body shifts from forming too many clots to bleeding out,” says Dr. Marcel Levi, a world-renowned hematologist and lead author on several DIC studies.
How Do Doctors Know? What is Disseminated Intravascular Coagulation testing?
Doctors don’t use a single test to define disseminated intravascular coagulation. Instead, they use a “scorecard” from the International Society on Thrombosis and Haemostasis (ISTH).
They look for four main red flags in your bloodwork:
- Low Platelet Count: You have fewer “plugging” cells.
- High D-Dimer: This shows your body frantically trying to break down the thousands of tiny clots it just made.
- Prolonged Clotting Time (PT/INR): Your blood takes way too long to form a solid clot.
- Low Fibrinogen: You have run out of the raw materials needed to stop a bleed.
If the score is 5 or higher, doctors confirm that disseminated intravascular coagulation is happening.
The 2026 Treatment Protocol: Calming the Storm
The primary answer to what is disseminated intravascular coagulation treatment is simple: Fix the original problem. If sepsis caused the DIC, doctors must give powerful antibiotics. If a pregnancy complication caused it, the baby must be delivered. Without stopping the “spark,” the fire will keep burning.
While fixing the cause, medical teams provide “supportive care”:
- Platelet Transfusions: They give you new “plugs” to stop the bleeding.
- Fresh Frozen Plasma (FFP): This replaces the missing proteins in your blood.
- Anticoagulants (Heparin): In rare cases where clotting is the main danger, doctors use blood thinners to stop the tiny dams from forming.
Expert Diagnostic Table: The ISTH Score
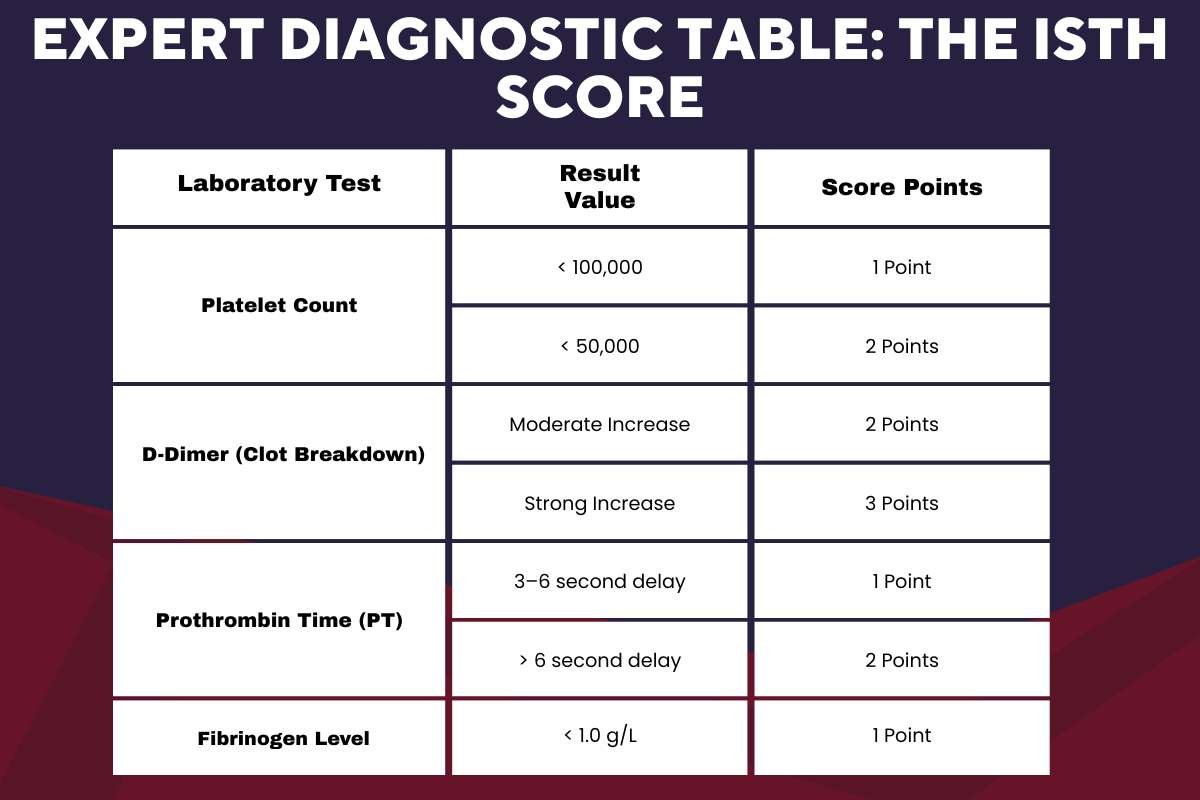
Doctors don’t guess. They use the ISTH Scoring System to determine DIC levels in a patient.
| Laboratory Test | Result Value | Score Points |
| Platelet Count | < 100,000 | 1 Point |
| < 50,000 | 2 Points | |
| D-Dimer (Clot Breakdown) | Moderate Increase | 2 Points |
| Strong Increase | 3 Points | |
| Prothrombin Time (PT) | 3–6 second delay | 1 Point |
| > 6 second delay | 2 Points | |
| Fibrinogen Level | < 1.0 g/L | 1 Point |
The Result: A score of 5 or higher confirms a diagnosis of overt disseminated intravascular coagulation.
A Real-Life Perspective: A Case Study Summary
A 2024 case study from Lablogatory described a 31-year-old woman with bleeding gums and bruising. Her bloodwork showed a classic DIC profile. Doctors quickly identified an underlying infection and started aggressive treatment. Because they caught it early, her body regained balance before her organs failed. This shows that knowing what is disseminated intravascular coagulation can save lives.
Symptoms You Should Never Ignore
Knowing disseminated intravascular coagulation means recognizing the early warning signs. Contact a doctor immediately if you or a loved one experiences:
- Unexplained bruising or small purple dots on the skin (petechiae).
- Bleeding from the gums or nose without a clear reason.
- Shortness of breath or chest pain.
- A sudden drop in urine output (a sign your kidneys are struggling).
Helpline Numbers & Support Networks
If you are facing a medical crisis or need support, these organizations provide expert guidance:
- Emergency (Global): Call 911 (US/Canada), 999 (UK), or 108 (India) immediately for active bleeding.
- National Blood Clot Alliance (NBCA): Call 1-877-4-NO-CLOT (1-877-466-2568) for patient guides and clotting education.
- Sepsis Alliance: Visit Sepsis.org for virtual support communities like Sepsis Alliance Connect.
- Blood Cancer United: Call 1-800-955-4572 for support if cancer triggered your blood disorder.
- Crisis Support (US): Dial 988 if the emotional toll of a medical crisis becomes overwhelming.
- Blood Availability (India): Call 94800 44444 (Project Disha) to find the nearest safe blood bank.
What to Do for Loved Ones: A Caregiver’s Guide

When a family member faces what is disseminated intravascular coagulation, you play a vital role in their recovery. Follow these steps to support them:
- Monitor the Skin: Watch for new purple spots or “oozing” from IV sites. Report these to the nurse immediately.
- Ask About the “ISTH Score”: Ask the doctor, “What is the current ISTH score?” This helps you track if the condition is improving.
- Advocate for the Root Cause: Ensure the medical team is aggressively treating the infection or injury that started the DIC.
- Limit Movement: Help the patient stay still to prevent accidental bumps or bruises that could lead to major internal bleeding.
- Seek Mental Health Support: DIC is a traumatic event. Use virtual communities like Sepsis Alliance Connect to talk with other families who survived this “blood storm.”
Summary:
So, what is disseminated intravascular coagulation in a nutshell? It is your body’s clotting system moving from “safe” to “overdrive.” It is a paradox where you clot and bleed at the same time.
By understanding disseminated intravascular coagulation, patients and families can ask better questions during a hospital stay. While the condition is scary, modern medicine has advanced scoring systems and blood products to help you pull through.
Final Fact:
Did you know that men and women have equal risks for DIC? However, obstetric complications make it a unique focus in women’s health. Regardless of gender, anyone facing a severe health crisis must be monitored for disseminated intravascular coagulation daily.
Now that you know what is disseminated intravascular coagulation, share this with someone who needs to understand the complexities of blood health.