The human body is a complex system composed of various bones, muscles, and connective tissues. This system works together to facilitate movement, support, and protection. In the lower limb, the tibia and fibula stand out as two essential bones that play a vital role in these functions. This extensive guide aims to delve deeper into the anatomy, functions, common injuries, treatment options, and preventive measures. It highlights the significance of the tibia and fibula in maintaining overall musculoskeletal health.
Anatomy of the Tibia and Fibula:
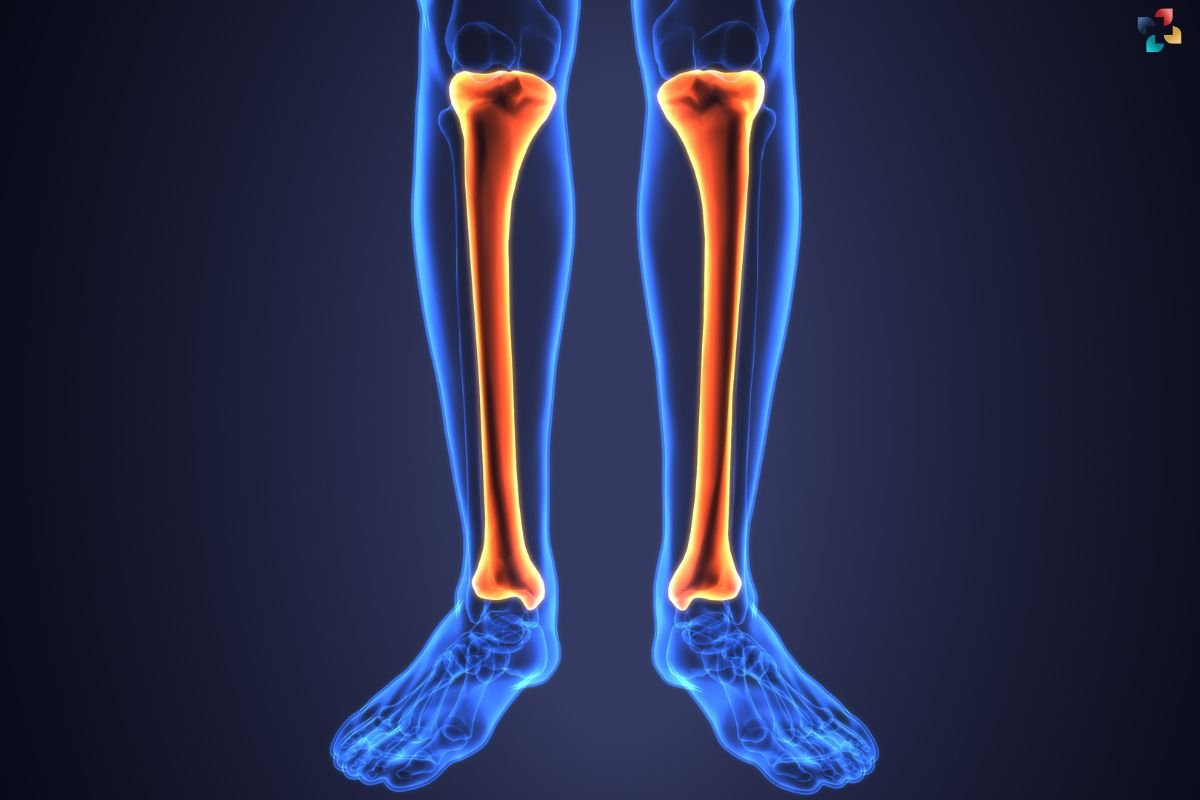
The tibia, also known as the shinbone, is the larger and stronger of the two bones in the lower leg. It is located medially (towards the midline of the body) and runs parallel to the fibula. Extending from the knee to the ankle, the tibia forms the primary weight-bearing bone of the lower leg. It articulates with the femur at the knee joint and the talus bone at the ankle joint, contributing to the stability and mobility of these joints.
In contrast, the fibula is the thinner, long bone located laterally (on the outer side) of the lower leg. Although it is not directly involved in weight-bearing, the fibula provides crucial support to the ankle joint and serves as an attachment site for several muscles and ligaments. The fibula articulates with the tibia proximally and with the tibia and talus distally, forming part of the ankle joint and enhancing its stability.
Functions:
1. Weight Bearing
The primary function of the tibia is to bear and distribute the body’s weight from the femur to the foot during standing, walking, running, and other weight-bearing activities. Its robust structure and alignment with the talus bone ensure efficient transmission of forces and maintain the integrity of the lower limb.
2. Muscle Attachment and Movement
Both the tibia and fibula serve as attachment points for various muscles, tendons, and ligaments that contribute to movement and stability. Muscles such as the quadriceps, hamstrings, gastrocnemius, soleus, and tibialis anterior exert their force through these bones to produce coordinated movements of the knee, ankle, and foot.
3. Joint Stability and Range of Motion
The bones work synergistically to provide stability to the ankle joint while allowing for a wide range of motion. The fibula’s role in resisting excessive lateral forces helps prevent ankle sprains and other injuries, while the tibia’s articulation with the femur and talus enables controlled movements such as dorsiflexion, plantarflexion, inversion, and eversion.
4. Shock Absorption and Force Distribution
The structure of the tibia, with its thick cortical bone and trabecular architecture, enables it to absorb and distribute forces generated during weight-bearing activities. This shock-absorbing capacity helps reduce the risk of fractures and soft tissue injuries, particularly during high-impact movements such as jumping or landing.
Common Injuries Associated with the Tibia and Fibula:
1. Fractures
Fractures of the tibia and fibula are prevalent injuries, often resulting from trauma such as falls, sports-related impacts, or motor vehicle accidents. Tibial fractures can occur at various locations along the bone, including the proximal (near the knee), shaft, or distal (near the ankle) regions, while fibular fractures are more common in the distal portion. Depending on the severity and displacement of the fracture fragments, treatment may involve casting, bracing, or surgical intervention to realign the bones and promote healing.
2. Ankle Sprains and Ligament Injuries
Ankle sprains are among the most common musculoskeletal injuries, involving stretching or tearing of the ligaments that support the ankle joint. In severe cases, these injuries may also affect the ligaments attached to the tibia and fibula, leading to instability and functional impairment. Treatment typically includes rest, ice, compression, and physical therapy to restore strength and flexibility to the affected ligaments and muscles.
3. Stress Fractures and Overuse Injuries
Stress fractures are small cracks or fissures that develop in the bones due to repetitive stress or overuse, often seen in athletes or individuals engaged in high-impact activities. The tibia is particularly susceptible to stress fractures, especially in the lower third of the bone (known as “shin splints”). Treatment involves rest, activity modification, and gradual return to activity to allow for adequate bone remodeling and healing.
4. Compartment Syndrome
Compartment syndrome is a serious condition that can occur following traumatic injury or exertional activities, resulting in increased pressure within the compartments of the lower leg. This elevated pressure can impede blood flow to the muscles and nerves, leading to tissue ischemia and nerve damage. Prompt recognition and treatment, including fasciotomy to relieve pressure, are essential to prevent long-term complications and preserve limb function.
Treatment Options for Tibia and Fibula Injuries:
1. Conservative Management
Many tibia and fibula injuries, such as non-displaced fractures or ligament sprains, can be effectively managed with conservative measures. This may include rest, immobilization with casting or bracing, ice therapy, elevation, and pain management with nonsteroidal anti-inflammatory drugs (NSAIDs). Physical therapy plays a crucial role in the rehabilitation process, focusing on restoring range of motion, strength, and functional mobility.
2. Surgical Intervention
In cases of severe fractures, displaced fractures, or ligamentous injuries that fail to respond to conservative treatment, surgical intervention may be necessary to realign the bones, stabilize the joint, or repair damaged tissues. Surgical techniques may involve internal fixation with plates, screws, intramedullary nails, external fixation devices, or ligament reconstruction procedures. The goal of surgery is to restore anatomical alignment, promote healing, and minimize the risk of long-term complications such as malunion, nonunion, or post-traumatic arthritis.
3. Rehabilitation and Physiotherapy
Rehabilitation following tibia and fibula injuries is essential to optimize functional outcomes, prevent complications, and facilitate return to pre-injury activities. Physiotherapy interventions focus on strengthening the surrounding muscles, improving joint range of motion, enhancing proprioception and balance, and gradually reintroducing weight-bearing activities. A structured rehabilitation program tailored to the individual’s specific injury, functional goals, and activity level is essential for achieving successful outcomes and minimizing the risk of recurrent injuries.
Preventing Tibia and Fibula Injuries:
While some tibia and fibula injuries are unavoidable, adopting preventive strategies can help reduce the risk of musculoskeletal problems and maintain overall lower limb health:
1. Warm-up and Cool-down
Engage in proper warm-up exercises before participating in physical activity to prepare the muscles, tendons, and ligaments for increased demand. Incorporate dynamic stretching, mobility drills, and light aerobic activity to improve blood flow and flexibility. Similarly, include a cool-down phase at the end of the workout to facilitate muscle recovery and prevent stiffness.
2. Gradual Progression and Cross-Training
Avoid sudden increases in training volume or intensity, as this can overwhelm the musculoskeletal system and increase the risk of overuse injuries. Gradually progress training loads, duration, and intensity over time, allowing adequate recovery between sessions. Incorporate cross-training activities such as swimming, cycling, or yoga to diversify movement patterns, reduce repetitive stress on specific structures, and enhance overall fitness and resilience.
3. Proper Footwear and Equipment

Choose appropriate footwear designed for your specific activity and foot type to provide adequate support, cushioning, and stability. Replace worn-out shoes regularly to maintain optimal shock absorption and foot alignment. Consider using orthotic inserts or ankle braces if you have underlying biomechanical issues or a history of ankle instability to enhance joint stability and reduce the risk of injuries.
4. Technique and Form
Pay attention to proper technique and biomechanics during exercise and sports activities to minimize excessive stress on the lower limb joints and soft tissues. Work with a qualified coach, trainer, or physical therapist to learn correct movement patterns, posture, and alignment principles. Focus on developing strength, flexibility, and neuromuscular control to improve movement efficiency and reduce the risk of compensatory injuries.
5. Listen to Your Body
Be mindful of your body’s signals and avoid ignoring pain, discomfort, or signs of fatigue. Rest and recover adequately between training sessions, allowing for tissue repair and adaptation. Incorporate rest days, active recovery activities, and periodization into your training schedule to prevent overtraining and burnout.
Conclusion:
The tibia and fibula are integral components of the lower limb, providing structural support, stability, and mobility essential for daily activities and athletic performance. Understanding the anatomy, functions, common injuries, treatment options, and preventive measures associated with these bones is crucial for maintaining musculoskeletal health and minimizing the risk of debilitating conditions. By adopting proactive strategies such as proper warm-up, gradual progression, technique refinement, and adequate recovery, individuals can safeguard the integrity of their tibia and fibula, enabling them to lead active, fulfilling lives free from lower limb injuries and limitations.