A U.K. lung transplant patient detected early organ rejection through a donor skin graft on his arm, enabling faster treatment, as researchers test a new method to identify Lung Transplant Rejection sooner and improve survival rates.
Patient Spots Early Rejection Through Donor Skin Patch
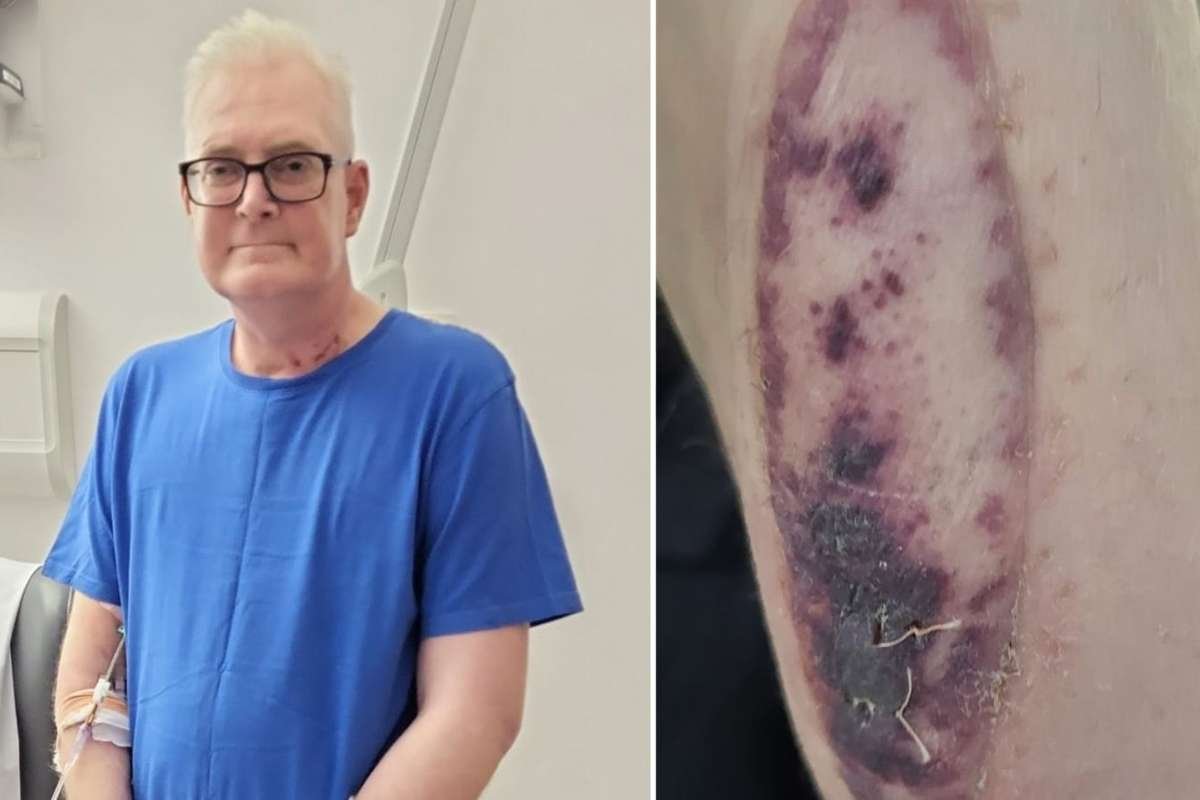
Darren White, 53, is among the first lung transplant patients in the United Kingdom to receive a donor skin graft designed to signal early organ rejection. The patch, placed on his forearm during surgery in late 2024, helped doctors intervene quickly when complications arose.
Three months after his transplant, White noticed a purple rash on the graft and sent photos to his medical team. Tests confirmed mild rejection of his new lung, and he was treated promptly with steroids.
“I definitely believe the skin patch helped to stop the lungs from being rejected,” White said. “I was feeling fine. The only sign was the rash.”
More than a year later, White said he is recovering well and has regained mobility, allowing him to spend more time with his three-year-old son.
Trial Tests Skin as Early Warning System for Transplants
The experimental procedure is part of the Sentinel trial led by experts in collaboration with NHS Blood and Transplant. The study involves grafting a small section of donor skin, about 10 centimeters by three centimeters, onto transplant recipients.
Researchers believe skin tissue shows signs of rejection earlier than internal organs and is easier to monitor visually. A visible rash on the graft can act as an early warning system, allowing treatment before significant organ damage occurs.
So far, 10 patients have received the grafts as part of the study. The trial aims to recruit 152 participants across five major transplant centers in England and will run through 2027.
Lung Transplant Rejection remains difficult to detect using traditional methods such as blood tests, biopsies, and X-rays. According to NHS Blood and Transplant, rejection occurs in nearly one-third of patients, most commonly within the first three to six months after surgery.
Researchers Aim to Reduce Organ Rejection Risks
Henk Giele, chief investigator of the trial and a plastic surgeon at the University of Oxford, said the approach could transform transplant monitoring if proven effective.
“It seems logical that having a window to your transplant can provide an early warning system of rejection,” Giele said. “But we have to prove it works.”
The graft procedure requires additional consent from donor families, coordinated by specialist nurses. Researchers say the willingness of families to support the trial has been critical.
Emma Lawson, innovation and research lead at NHS Blood and Transplant, said the project highlights the impact of donor generosity. “Patients are now receiving these grafts, and we are privileged to work alongside them to enable this important trial,” she said.
White, a former bus driver from Stockton-on-Tees, said he hopes the study will benefit future transplant patients.
Lung Transplant Rejection is the biggest fear of any transplant recipient,” he said. “Anything that can catch it earlier is worth it.”