Have you ever wondered why the most popular Google search term in 2026 is “ADD vs ADHD”? Millions of people struggle with this outdated confusion, so you’re not alone. The term “ADD,” which was once used to describe attention problems without hyperactivity, is no longer relevant. In psychiatric manuals such as the DSM-5, ADHD is the official diagnosis for inattentive, hyperactive-impulsive, and combined types. ADD vs ADHD: Key Differences Most People Don’t Know Revealed
Children and adults struggle as a result of this confusion, which delays diagnosis and treatment. Discover the true distinctions, important symptoms, ADHD subtypes, and how to receive an accurate diagnosis in this guide, clearing the fog once and for all.
What is ADD?
In 1980, the DSM-III introduced Attention Deficit Disorder (ADD) as the new name for what was previously called “Hyperkinetic Reaction of Childhood.” This shift emphasized attention deficits over hyperactivity alone. ADD included two subtypes: ADD with hyperactivity (restless, impulsive behaviors) and ADD without hyperactivity (primarily inattention, daydreaming, and disorganization).
The term highlighted core struggles like poor focus and distractibility, affecting school and daily life.
ADD became outdated due to advances in neuroscience and behavioral research, revealing hyperactivity, impulsivity, and inattention as interconnected. In 1987, the DSM-III-R replaced it with ADHD, unifying criteria in modern manuals like DSM-5.
ADD Timeline
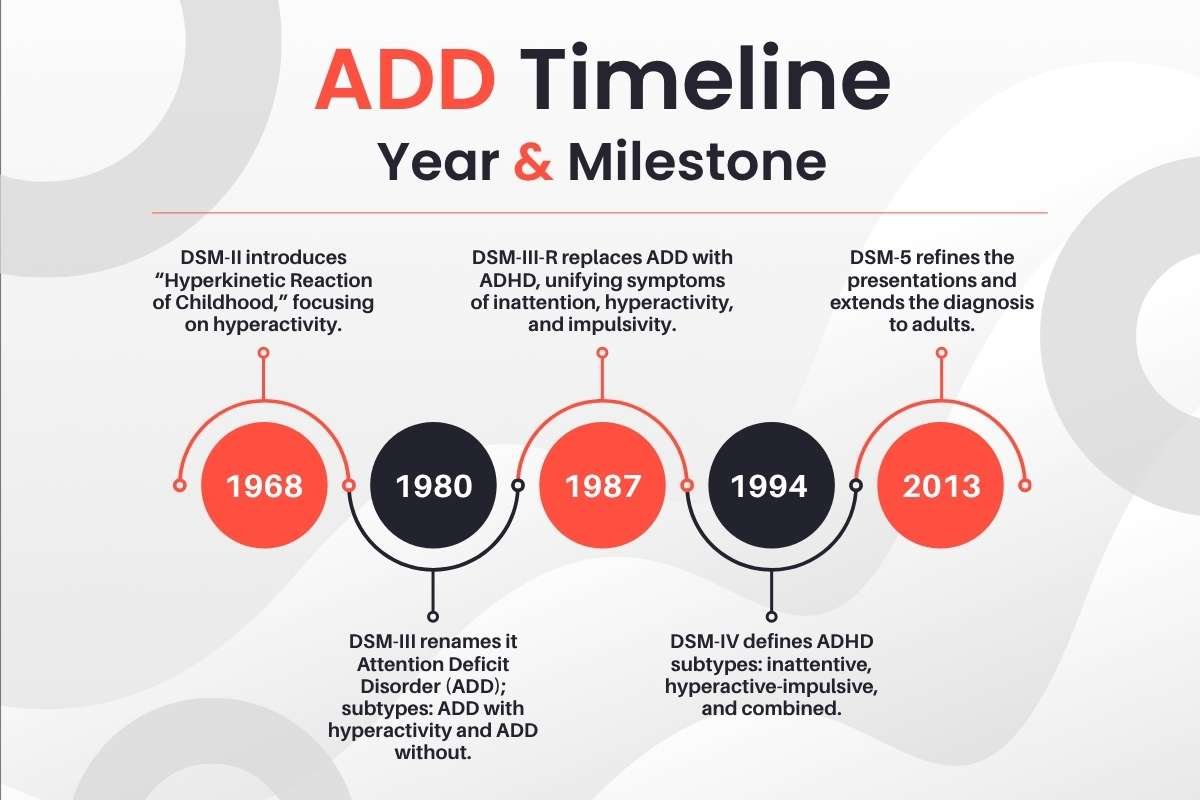
| Year | Milestone |
| 1968 | DSM-II introduces “Hyperkinetic Reaction of Childhood,” focusing on hyperactivity. |
| 1980 | DSM-III renames it Attention Deficit Disorder (ADD); subtypes: ADD with hyperactivity and ADD without. |
| 1987 | DSM-III-R replaces ADD with ADHD, unifying symptoms of inattention, hyperactivity, and impulsivity. |
| 1994 | DSM-IV defines ADHD subtypes: inattentive, hyperactive-impulsive, and combined. |
| 2013 | DSM-5 refines the presentations and extends the diagnosis to adults. |
What is ADHD?
ADHD, or Attention-Deficit/Hyperactivity Disorder, is a neurodevelopmental disorder that impairs attention, impulse control, and activity regulation. Defined in the DSM-5, it manifests through three core symptom clusters: inattention (trouble focusing, disorganization, forgetfulness), hyperactivity (excessive movement, fidgeting, restlessness), and impulsivity (acting without thinking, interrupting others).
Symptoms like difficulty sustaining focus, impulsive decisions, and constant restlessness define ADHD. It affects children (often diagnosed early), adolescents (intensifying social challenges), and adults (impacting work and relationships).
Proper recognition across life stages enables targeted interventions.
ADD vs ADHD: The Real Difference
For many years, people used ADD and ADHD interchangeably, which created confusion. In reality, ADD is an outdated term, while ADHD is the official medical diagnosis used today. Modern psychiatry now classifies attention disorders under one umbrella condition called Attention-Deficit/Hyperactivity Disorder.
The terminology changed when the Diagnostic and Statistical Manual of Mental Disorders, published by the American Psychiatric Association, standardized ADHD as the official diagnosis. What people used to call ADD is now considered a specific presentation of ADHD.
Comparison: ADD vs ADHD
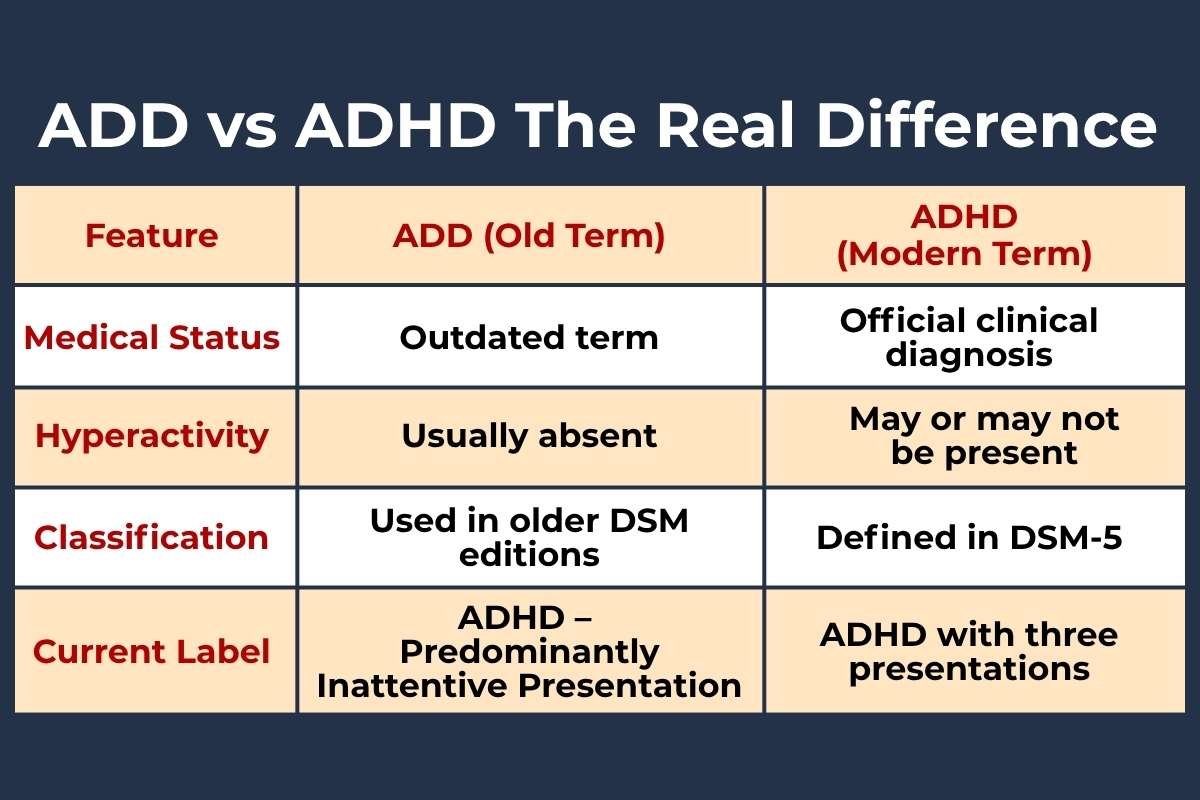
| Feature | ADD (Old Term) | ADHD (Modern Term) |
| Medical Status | Outdated term | Official clinical diagnosis |
| Hyperactivity | Usually absent | May or may not be present |
| Classification | Used in older DSM editions | Defined in DSM-5 |
| Current Label | ADHD – Predominantly Inattentive Presentation | ADHD with three presentations |
What was once called ADD is now known as ADHD – Predominantly Inattentive Presentation, where individuals mainly struggle with focus, attention, and organization rather than hyperactivity.
Experts consider ADD an outdated label, and modern medical guidelines now use ADHD as the official umbrella diagnosis, helping ensure accurate understanding, diagnosis, and treatment.
The Three Types of ADHD:
Understanding these distinctions helps clinicians and educators provide targeted support based on the specific challenges an individual faces.
1. Predominantly Inattentive Presentation
Formerly known as ADD, this presentation is often overlooked because the symptoms are internal rather than disruptive. Individuals may appear quiet or “spacey” rather than hyperactive.
- Daydreaming: Often loses focus during conversations or tasks, appearing to be in their own world.
- Forgetfulness: Frequently loses daily items like keys, phones, or school assignments.
- Poor Organization: Struggles with time management, breaking down large projects, or maintaining a tidy workspace.
2. Predominantly Hyperactive-Impulsive Presentation
This is the “classic” image of ADHD, characterized by a high need for movement and difficulty with self-regulation.
- Restlessness: A constant internal “motor” that makes sitting still for long periods (like in a meeting or classroom) feel physically uncomfortable.
- Interrupting Others: Difficulty waiting for a turn in conversation, often finishing others’ sentences or blurting out answers.
- Difficulty Waiting: High levels of impatience in lines or during activities that require a slow pace.
3. Combined Presentation
This is the most common diagnosis. It occurs when an individual meets the diagnostic threshold for both inattention and hyperactivity-impulsivity.
- Overlapping Symptoms: A person may struggle with organizing their schedule (inattentive) while also finding it impossible to sit through a movie (hyperactive).
- Dynamic Nature: Symptoms can shift. A child might present as Combined, but as an adult, the physical hyperactivity may diminish into internal restlessness while the inattentive symptoms persist.
ADD vs ADHD Symptoms in Children vs Adults:

ADHD symptoms evolve but often persist from childhood into adulthood, impacting daily functioning.
In Children
Youngsters show clear signs, such as trouble staying seated in class, difficulty focusing during lessons, and interrupting teachers or peers impulsively. These behaviors disrupt school and social interactions.
In Adults
Challenges shift to chronic disorganization (cluttered spaces, lost items), poor time management (chronic lateness), and difficulty completing long tasks (procrastination on work projects). Restlessness may be internalized as mental unease.
Many children with ADHD continue experiencing symptoms as adults, though they may adapt coping strategies. Early recognition improves lifelong management.
How is ADHD Diagnosed?
An accurate ADHD diagnosis is a comprehensive process, as there is no single medical test (like a blood test or brain scan) to confirm the condition. Instead, clinicians follow a multi-step evaluation to ensure diagnostic accuracy and align with EEAT medical authority standards.
The Diagnostic Process
- Behavioral Assessment: Using standardized rating scales to measure symptom frequency.
- Medical History: Reviewing developmental milestones and family history to identify genetic patterns.
- DSM-5-TR Criteria: Clinicians verify if the patient meets the official symptom threshold for Inattentive, Hyperactive, or Combined presentations.
- Collateral Input: Gathering observations from parents, teachers, or partners to see how symptoms manifest in different environments.
- Differential Diagnosis: Ruling out conditions with overlapping symptoms, such as anxiety, sleep disorders, or learning disabilities.
According to global clinical standards. A formal diagnosis requires symptoms to persist for at least six months. Crucially, these traits must appear in multiple settings. Such as both school and home. This can significantly impair daily functioning.
Common Myths About ADD vs ADHD:
Misconceptions persist despite clear medical consensus. Here’s the truth behind popular myths.
Myth 1: ADD and ADHD are completely different disorders
Fact: In discussions about ADD vs ADHD, it’s important to know that ADD is an outdated term for what is now ADHD’s predominantly inattentive presentation. Modern DSM-5 unifies them under one diagnosis.
Myth 2: ADHD only affects children
Fact: Symptoms often continue into adulthood, though they may shift (e.g., hyperactivity becomes inner restlessness). About 60% of children retain diagnoses as adults.
Myth 3: Hyperactivity is always present
Fact: The inattentive type lacks obvious hyperactivity, focusing on issues like forgetfulness and disorganization, why ADD was once used.
Myth 4: ADHD is caused by bad parenting
Fact: It’s a neurodevelopmental disorder with genetic and brain structure factors, not parenting. The environment plays a minor role.
Debunking these empowers an accurate understanding and treatment.
Global ADHD Statistics and Prevalence:
ADHD impacts millions worldwide, with varying prevalence across ages and regions.
Children
Around 7.2% of children globally (roughly 129 million) have ADHD, per meta-analyses of 175 studies. In the U.S., about 6.5 million children (10.5%) carry a current diagnosis.
Adults
U.S. data shows 6.0% of adults (15.5 million) diagnosed, up from prior estimates. Globally, adult prevalence ranges from 3.1% to 6.76%, affecting 366 million people.
Rates vary: highest in countries like Haiti (2.7%) and lowest in parts of Asia (0.6%). Many adults remain undiagnosed, with rising recognition driving increases. Combined U.S. cases total 22 million.
Treatment and Management Options:

Effective ADHD treatment combines therapies, medications, and lifestyle strategies, tailored after a professional diagnosis. Understanding ADD vs ADHD clarifies that modern inattentive ADHD (once called ADD) responds well to these approaches.
- Behavioral Therapy: Teaches coping skills, organization, and impulse control. Ideal for children and adults to build routines.
- Medication: Stimulants (e.g., methylphenidate) or non-stimulants boost focus and reduce hyperactivity. Prescribed by specialists after evaluation.
- Cognitive Behavioral Therapy (CBT): Targets negative thought patterns, improving time management, and self-esteem.
- Lifestyle Changes: Prioritize sleep (7-9 hours), regular exercise (30 min daily), and structured routines. Nutrition and mindfulness also help sustain attention.
Always seek a professional diagnosis first. Self-treatment risks mismanagement. Multimodal plans yield the best results.
When to Seek Professional Help?
Recognize ADHD signs early to prevent worsening impacts on life. Persistent symptoms across settings signal the need for evaluation.
Key Signs
- Ongoing attention problems, like chronic forgetfulness or inability to focus.
- Academic struggles (failing grades despite effort) or work difficulties (missed deadlines).
- Impulsive or disruptive behavior, such as constantly interrupting or making risky decisions.
Who to Consult
- Psychiatrists: For diagnosis and medication management.
- Psychologists: Behavioral assessments and therapy.
- Pediatricians: Initial screening for children.
- ADHD Specialists: Comprehensive evaluations and tailored plans.
Prompt help improves outcomes. Don’t delay if symptoms impair daily functioning.
Conclusion:
In today’s medical science, ADD vs ADHD is often misunderstood, as ADD and ADHD are just two different names for the same thing. ADD is an old term from the DSM-III from the 1980s that is now part of ADHD, which is the current diagnosis in DSM-5 and around the world.
ADHD features three presentations: predominantly inattentive (what was once called ADD), predominantly hyperactive-impulsive, and combined.
Getting diagnosed early opens up behavioral therapy, medication, and lifestyle changes that can help people of all ages focus better, get along with others, and be more successful.
If you or someone you care about is confused about ADD vs. ADHD, see a professional. Better management and empowered living come from having a clear understanding.
FAQ:
Why ADD was renamed ADHD?
The term ADD was replaced in 1987 when researchers recognized that attention disorders often include a broader range of symptoms, such as impulsivity and hyperactivity. To better reflect these patterns, medical experts adopted ADHD as the unified diagnostic category.
What causes ADHD?
The exact cause of ADHD is not fully understood, but research suggests a combination of factors, including genetics, brain structure differences, and environmental influences. Family history is considered one of the strongest risk factors.
Can ADHD be treated or managed?
Yes. While ADHD has no permanent cure, it can be effectively managed with treatment options such as behavioral therapy, medication, lifestyle adjustments, and structured routines. Early diagnosis and proper support significantly improve outcomes for both children and adults.